How Sleep Apnea and Hypertension Impact Your Health
At the Center for Dental Sleep Health in Nashua, NH, Dr. Stephen Ura addresses the intricate relationship between sleep apnea and hypertension. These interconnected conditions can significantly impact your health, but with proper diagnosis and treatment, you can improve your quality of life.
Contact our Nashua, NH, dental office today at (603) 886-4300 to learn more about the connection between these conditions and why diagnosing and treating both is vital.


The Sleep Apnea-Hypertension Connection
Sleep apnea, characterized by breathing interruptions during sleep, and hypertension (high blood pressure) often coexist, each potentially worsening the other. Recent studies show that 30 to 50 percent of people with hypertension also have sleep apnea, highlighting the importance of addressing both conditions simultaneously.
Key Symptoms to Watch For
Recognizing the signs of sleep apnea and hypertension is crucial for early intervention. Be aware of these common symptoms:
- Loud snoring
- Daytime fatigue
- Morning headaches
- Difficulty concentrating
- Elevated blood pressure readings


How Sleep Apnea Affects Blood Pressure
Sleep apnea can impact your blood pressure through several mechanisms:
- Triggers Sympathetic Nervous System Activation: Frequent breathing interruptions cause stress responses, increasing heart rate and constricting blood vessels, which raises blood pressure.
- Increases Inflammation and Oxidative Stress: Repeated oxygen level drops lead to inflammation and the production of harmful free radicals, damaging blood vessel walls and promoting hypertension.
- Contributes to Endothelial Dysfunction: Sleep apnea can impair the inner lining of blood vessels, reducing their ability to dilate and regulate blood pressure effectively.
- May Lead to Insulin Resistance: Sleep disruptions can affect glucose metabolism, potentially leading to insulin resistance, which is associated with increased blood pressure.
Diagnostic Approaches
Sleep Apnea Diagnosis
Accurate diagnosis of sleep apnea is essential for effective management. Polysomnography, commonly referred to as a sleep study, is the gold standard for diagnosing sleep apnea. This comprehensive test monitors various physiological parameters during sleep, including airflow, oxygen levels, and brain activity. Home sleep apnea testing, which involves portable monitoring devices, may be suitable for some individuals with suspected sleep apnea.
Hypertension Diagnosis
Diagnosing hypertension involves measuring blood pressure levels. Regular blood pressure measurements are crucial for identifying sustained hypertension. Ambulatory blood pressure monitoring, which involves wearing a portable blood pressure monitor over 24 hours, provides a more comprehensive assessment of blood pressure variations throughout the day and night. Accurate diagnosis is the foundation for developing targeted treatment strategies.

Treatment Strategies

Lifestyle Modifications
- Weight Loss: Achieving and maintaining a healthy weight can significantly reduce the severity of sleep apnea and lower blood pressure levels. Lifestyle changes, including a balanced diet and regular exercise, play a crucial role in weight management.
- Exercise: Regular physical activity has been shown to improve both sleep apnea and hypertension. Aerobic exercises, such as walking or cycling, can contribute to weight loss and enhance cardiovascular health.
- Dietary Changes: Dietary modifications, such as reducing salt intake and adopting the DASH (Dietary Approaches to Stop Hypertension) diet, can help manage hypertension. These changes may also have positive effects on sleep apnea severity.
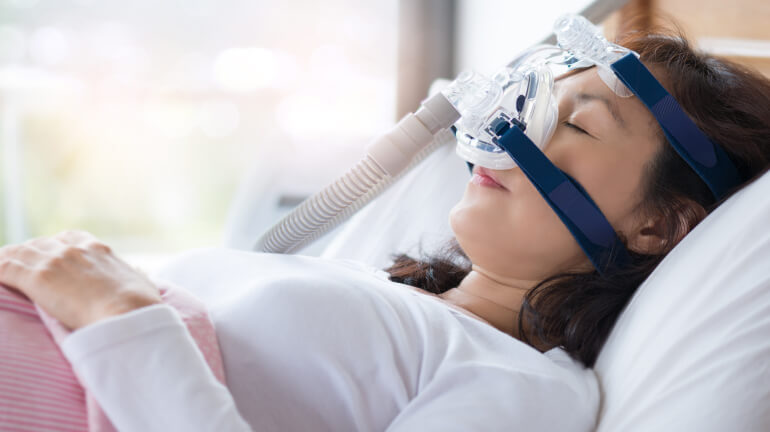
Continuous Positive Airway Pressure (CPAP) Therapy
Continuous positive airway pressure, or CPAP, is a widely used and effective treatment for obstructive sleep apnea. It involves wearing a mask over the nose or nose and mouth during sleep, delivering a continuous stream of air to keep the airway open. CPAP not only improves sleep apnea symptoms but can also positively impact blood pressure control.

Oral Appliance Therapy
Mandibular Advancement Devices (MADs) are oral appliances that reposition the lower jaw and tongue to keep the airway open during sleep. They’re considered an effective alternative to CPAP, especially for individuals with mild to moderate obstructive sleep apnea or those who cannot tolerate CPAP.

Pharmacological Interventions
- Antihypertensive Medications: Individuals with both sleep apnea and hypertension may benefit from antihypertensive medications. However, healthcare providers must carefully select medications, considering potential interactions with sleep apnea treatments.
- Medications for Sleep Apnea: Some medications, such as acetazolamide, may be prescribed to stimulate ventilation and improve respiratory function during sleep. However, the use of these medications is typically reserved for specific cases and should be closely monitored.
Frequently Asked Questions
Can treating sleep apnea lower my blood pressure?
Yes, effectively managing sleep apnea often leads to improved blood pressure control. Studies show that consistent CPAP use can reduce blood pressure by two to 10 mmHg.
How does sleep apnea affect heart health beyond hypertension?
Sleep apnea is associated with an increased risk of atrial fibrillation, heart failure, and coronary artery disease. Managing sleep apnea can significantly improve overall cardiovascular health.
Can certain foods help manage both sleep apnea and hypertension?
Yes, foods rich in potassium (like bananas and avocados) and those high in nitrates (such as leafy greens) can help lower blood pressure. Additionally, maintaining a healthy weight through proper nutrition can improve sleep apnea symptoms.
Can children have both sleep apnea and hypertension?
Yes, although less common, children can experience both sleep apnea and hypertension. Obesity, adenotonsillar hypertrophy, and certain medical conditions may contribute to the development of sleep apnea in children, which, if left untreated, can impact blood pressure.
Take Control of Your Health Today!
If you or someone you know is struggling with sleep apnea and hypertension, it’s time to take proactive steps toward a healthier life. Contact our Nashua, NH, dental office today at (603) 886-4300 or fill out our online contact form to schedule your appointment! We welcome new and existing patients in Hudson, Merrimack, and Milford, NH.
